The Importance of Breast Cancer Screening
Breast cancer is one of the most common types of cancer among women worldwide. Early detection through regular screening is crucial for improving treatment outcomes and reducing mortality rates. Breast cancer screening aims to identify the disease in its early stages, often before symptoms appear, when treatment is most effective. By understanding the importance of breast cancer screening and the various methods available, women can take proactive steps to protect their health and well-being.

Symptoms of Breast Cancer
While the primary goal of breast cancer screening is to detect the disease before symptoms develop, it's essential for women to be aware of the potential signs and symptoms of breast cancer. These may include:
- A lump or thickening in the breast or underarm area
- Changes in the size, shape, or appearance of the breast
- Dimpling, puckering, or redness of the breast skin
- Nipple changes, such as inversion, discharge, or scaliness
- Pain or tenderness in the breast, although this is less common
It's important to note that these symptoms can also be caused by benign (non-cancerous) conditions. However, if you experience any of these symptoms, it's crucial to consult your healthcare provider for a proper evaluation.
Breast Self-Examination
Breast self-examination (BSE) is a technique that women can use to familiarize themselves with the normal appearance and feel of their breasts, making it easier to detect any changes or abnormalities. While BSE is not considered a substitute for professional screening, it can be a valuable tool for women to take an active role in their breast health.
To perform a breast self-examination:
- Stand in front of a mirror with your arms at your sides, then raised overhead. Look for any changes in the size, shape, or appearance of your breasts.
- Feel your breasts while lying down, using the pads of your fingers in a circular motion. Cover the entire breast area, including the armpits.
- Gently squeeze the nipples to check for any discharge.
- Repeat the process while standing or sitting, ideally in the shower when the skin is wet and slippery.
If you notice any lumps, changes, or other concerning findings during your BSE, contact your healthcare provider for further evaluation.
The frequency of breast self-examination is a topic of ongoing discussion in the medical community. Some organizations recommend that women perform BSE monthly, typically a few days after the end of their menstrual period when the breasts are less tender and swollen. However, other organizations emphasize the importance of breast self-awareness, encouraging women to become familiar with the normal look and feel of their breasts and to report any changes to their healthcare provider, without necessarily adhering to a strict monthly schedule.
Ultimately, the decision to perform regular BSE should be made in consultation with your healthcare provider, taking into account your individual risk factors and personal preferences. Remember, BSE is not a substitute for professional screening, such as mammograms or clinical breast exams, but rather a complementary tool for detecting potential abnormalities between scheduled screenings.
Clinical Breast Examination
A clinical breast examination (CBE) is a physical exam performed by a healthcare provider, typically during an annual check-up or gynecological visit. During a CBE, the provider will:
- Visually inspect the breasts for any changes in size, shape, or symmetry
- Palpate (feel) the breasts, underarm areas, and the area above the collarbone for any lumps, thickening, or other abnormalities
- Assess any skin changes, nipple discharge, or other visible signs of concern
If the provider detects any abnormalities during the CBE, they may recommend additional testing, such as a mammogram, ultrasound, or biopsy, to further evaluate the findings.
Mammography
Mammography is the primary screening tool for detecting breast cancer in its early stages. A mammogram is an X-ray image of the breast that can reveal tumors or other abnormalities that may be too small to detect through physical examination.
There are two types of mammograms:
- Screening mammograms: These are routine exams performed on women with no symptoms or signs of breast cancer. The goal is to detect the disease early, when treatment is most effective.
- Diagnostic mammograms: These are performed when a woman has symptoms of breast cancer, such as a lump or nipple discharge, or when an abnormality is detected on a screening mammogram. Diagnostic mammograms typically involve more images and may take longer than screening mammograms.
Current guidelines recommend that women at average risk for breast cancer begin annual screening mammograms at age 45, with the option to start as early as age 40. Women aged 55 and older may transition to biennial (every two years) screening, depending on their individual risk factors and preferences. Women at higher risk for breast cancer, such as those with a family history of the disease or certain genetic mutations, may require earlier or more frequent screening.
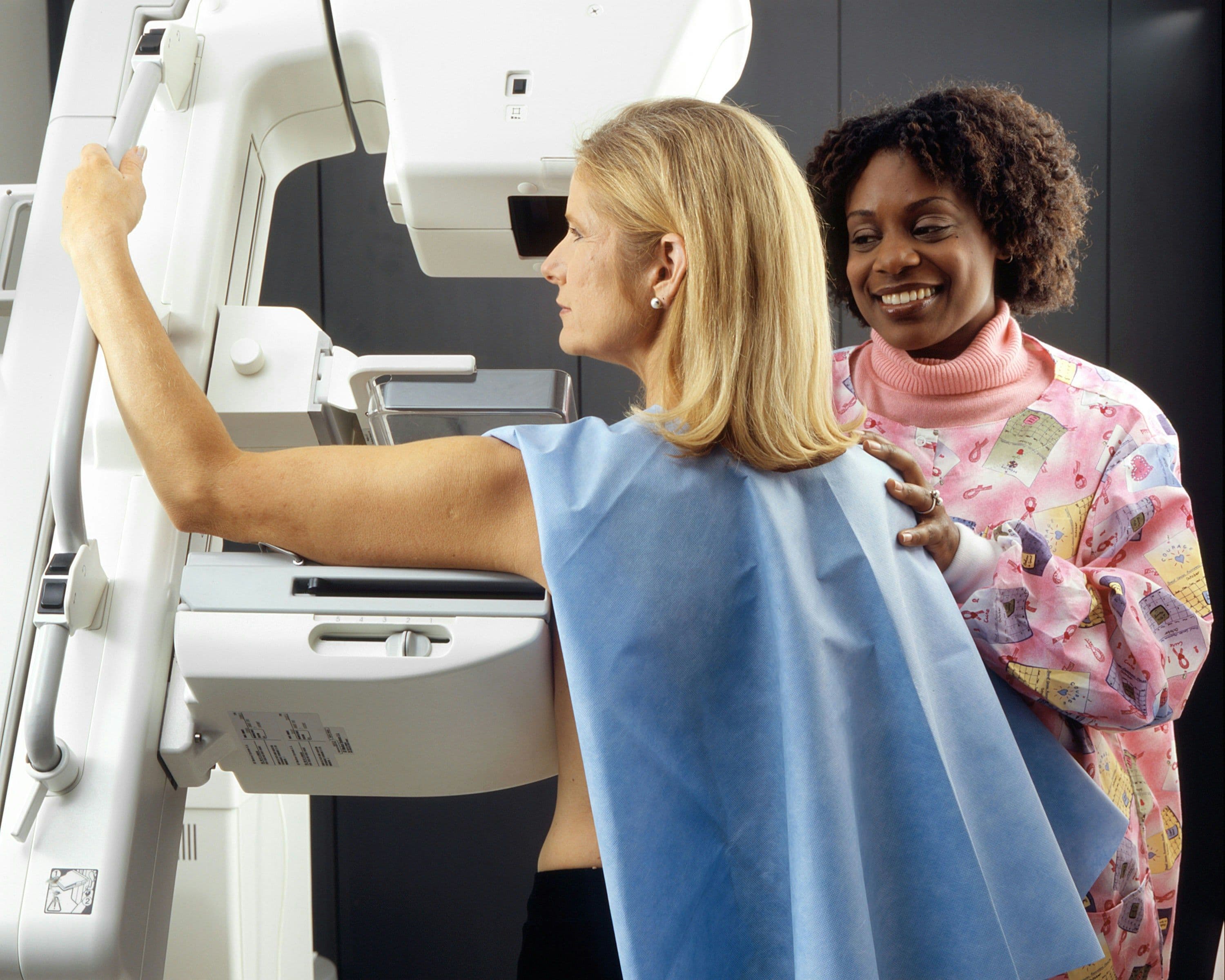
During a mammogram, you will stand in front of an X-ray machine designed specifically for breast imaging. A trained technologist will position your breast on a platform and gradually compress it with a clear plastic paddle. Compression is necessary to spread out the breast tissue, reducing the amount of radiation needed and providing a clearer image. You may feel some discomfort or pressure during the compression, but this is typically brief and tolerable.
The technologist will take images of each breast from different angles, usually two views per breast (top-to-bottom and side-to-side). You may be asked to hold your breath for a few seconds while each image is taken to minimize movement and ensure a clear picture. The entire procedure typically takes about 20-30 minutes.
After the mammogram, a radiologist will review the images and report the results to your healthcare provider. If any abnormalities are detected, you may be called back for additional imaging or tests, such as a diagnostic mammogram, ultrasound, or biopsy. It's important to remember that most callbacks do not result in a cancer diagnosis and are often due to benign findings or the need for clearer images.
Other Screening Methods
In addition to mammography, there are other screening methods that may be used in certain situations or for women at higher risk of breast cancer:
- Breast ultrasound: An imaging test that uses sound waves to create pictures of the breast tissue. Ultrasound can help distinguish between solid masses (which may be cancerous) and fluid-filled cysts (which are usually benign).
- Breast MRI: A detailed imaging test that uses magnets and radio waves to create cross-sectional pictures of the breast. MRI may be recommended for women at very high risk of breast cancer, such as those with a known genetic mutation or a strong family history of the disease.
- Molecular breast imaging (MBI): A newer test that uses a radioactive tracer and special camera to detect breast cancer. MBI may be used in addition to mammography for women with dense breast tissue, which can make it harder to detect tumors on a standard mammogram.
Your healthcare provider can help determine which screening methods are most appropriate for you based on your individual risk factors, breast tissue density, and personal preferences.
Conclusion
Regular breast cancer screening is a crucial component of women's health and well-being. By understanding the various screening methods available, such as breast self-examination, clinical breast exams, and mammography, women can take proactive steps to detect breast cancer in its earliest stages, when treatment is most effective. If you have any questions or concerns about your breast health or screening schedule, don't hesitate to discuss them with your healthcare provider. Remember, early detection saves lives – prioritize your breast health today.